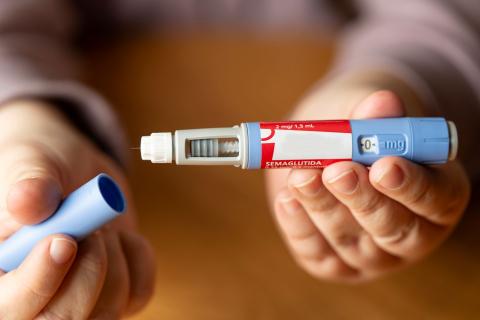
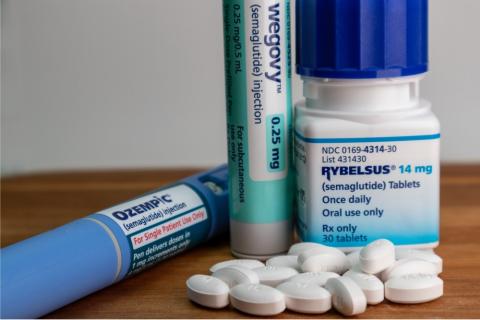
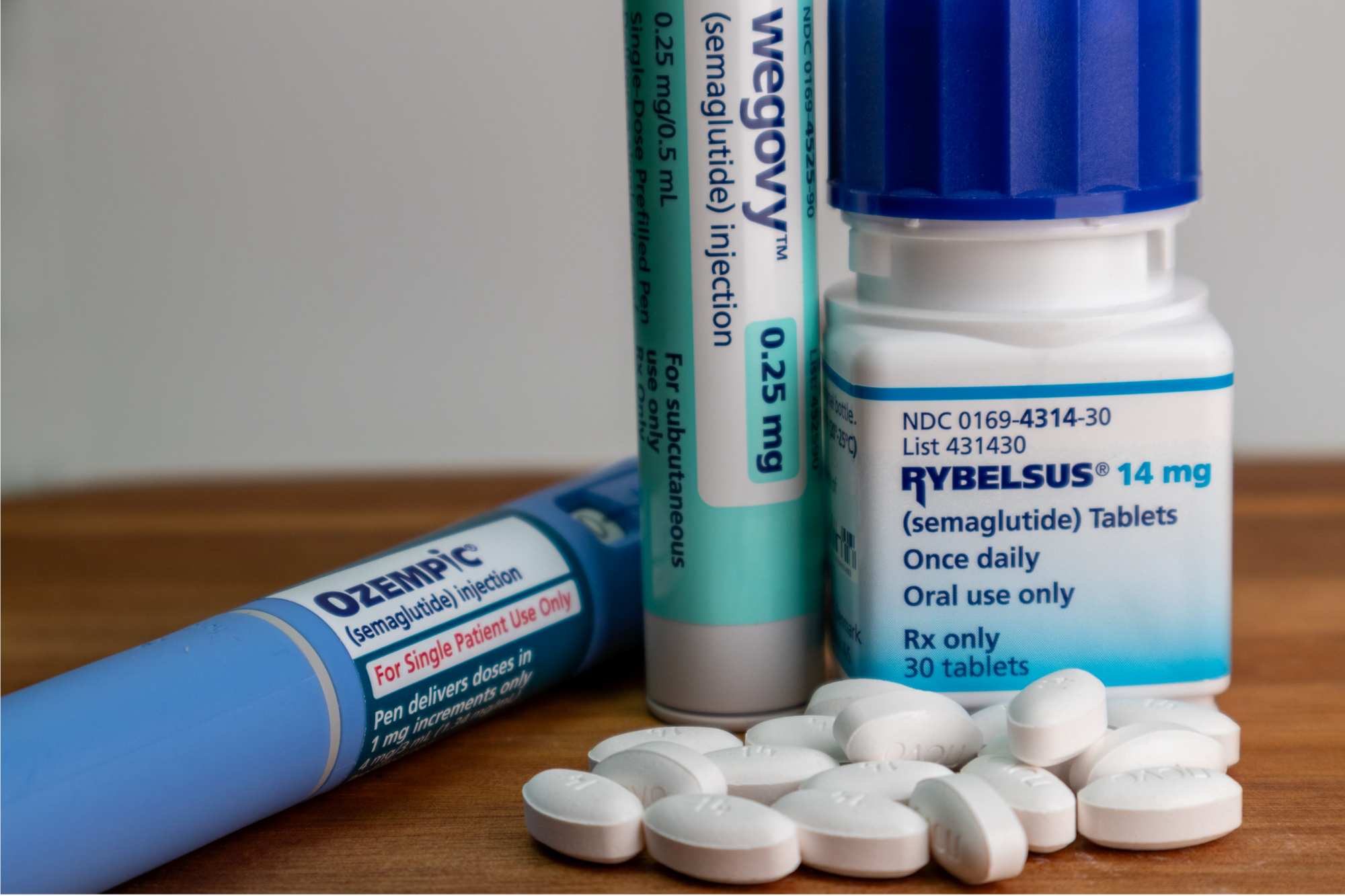
Oral semaglutide does not slow the progression of Alzheimer's disease, according to a trial
Oral semaglutide is not effective in slowing the progression of the disease in patients with mild Alzheimer’s disease, according to the findings of the first large-scale, randomised phase 3 clinical trials published in The Lancet. In these trials, around 3,800 patients aged between 55 and 85 with a confirmed diagnosis and mild symptoms received up to 14 mg daily of oral semaglutide or a placebo. After two years, no significant difference in disease progression was observed.
Cristóbal Morales - semaglutida alzhéimer
Cristóbal Morales
Head of the Metabolic Health, Diabetes and Obesity Unit at Vithas Hospital in Seville and member of the Spanish Society for the Study of Obesity (SEEDO)
Here, the news would be that the primary objective—the beneficial effect—was not achieved, unlike what has been seen with semaglutide in other indications. The key point is the lack of positive results, which does not invalidate the hypothesis. We still believe that neuroinflammation—that chronic, low-grade inflammation—may play a role in diseases such as Alzheimer’s. Experimental data had seemed to point in that direction.
This hypothesis is what led to the launch of this clinical trial, in which no benefit has been demonstrated. The study involved a population with early-stage Alzheimer’s disease, but with a low proportion of diabetes and obesity. We need to continue researching this highly prevalent disease.
Science is built through errors, and negative results are also valuable. Perhaps we should assess whether, in people with diabetes, high cardiovascular risk, and chronic low-grade inflammation, this type of treatment might have some benefit.
In summary, this is simply one result—one piece of data—that should encourage continued research into the neuroinflammation hypothesis, to explore potential solutions that could benefit the many people affected by this disease.
Diego Bellido - semaglutida alzhéimer
Diego Bellido
Head of the Endocrinology and Nutrition Department at the Ferrol Hospital Complex (CHUF) and President of the Spanish Society for Obesity (SEEDO)
Does the press release accurately reflect the study?
“Yes, in essence it does. It correctly conveys that oral semaglutide did not slow the clinical progression of early Alzheimer’s, although there were changes in biomarkers that did not translate into clinical benefit. The potential bias lies in oversimplifying these nuances.”
Is the study of good quality?
“Yes. It is a methodologically robust piece of work: two phase 3 trials, randomized, double-blind, placebo-controlled, with 3,808 participants across 566 centers in 40 countries. The main conclusion is well supported because the primary endpoint was clearly negative in both trials.”
How does this work fit with the existing evidence?
“It fits as a study that tempers previous enthusiasm. Preclinical and observational evidence, as well as some small studies, suggested potential benefits of GLP-1 agonists, but this large trial does not confirm clinical efficacy in early Alzheimer’s.”
Have the authors taken confounding factors into account? Are there important limitations?
“Yes, reasonably so. They adjusted for relevant variables in the analysis and the design was solid. Still, there are limitations: higher dropout rates due to adverse effects in the semaglutide group, possible unblinding due to gastrointestinal side effects and weight loss, and the cerebrospinal fluid (CSF) sub-study was much smaller than the main trial.”
What are the real-world implications?
“The practical implication is clear: these data do not support using 14 mg oral semaglutide to slow early Alzheimer’s. It may still be useful for obesity or diabetes, but its benefits should not be extrapolated to disease-modifying treatment for Alzheimer’s.”
Xavier Morató - semaglutida alzhéimer
Xavier Morató
Director of Clinical Trials at Ace Alzheimer Center Barcelona
The EVOKE and EVOKE+ studies were based on the hypothesis that the semaglutide-mediated impact on neuroinflammation could reduce disease progression in patients with Alzheimer’s disease (AD). Real-world evidence with semaglutide indicated that its use in patients with type 2 diabetes was associated with a lower risk of dementia, suggesting possible neuroprotective effects beyond glycemic control. These findings provided an important basis for further investigating semaglutide as a strategy to reduce dementia risk.
Metabolic conditions in midlife, such as obesity and diabetes, are well-established and modifiable risk factors for the development of dementia (as highlighted by the Lancet Commission on dementia risk factors). Excess adiposity and impaired glucose metabolism contribute to chronic inflammation, vascular dysfunction, and other pathophysiological mechanisms involved in neurodegeneration and cognitive decline. Taken together, this evidence supports evaluating semaglutide as a therapeutic approach to mitigate dementia risk and improve long-term brain health.
In the EVOKE studies, the mean age was 72.2 years. One could hypothesize that these interventions should be applied earlier in life. At the same time, since not all participants tolerated the highest dose of 14 mg and consequently received 3 or 7 mg during the study, a better understanding of the relationship between dosage and changes in Alzheimer’s disease biomarkers would help interpret the results more accurately. The 14 mg oral dose is equivalent to a weekly subcutaneous administration of 0.5 mg.
Finally, these patients were amyloid-positive, and it may be necessary to combine amyloid clearance with treatment using GLP-1 agonists to observe an effect. Alternatively, these treatments might be effective at earlier stages, in patients at higher risk of amyloid accumulation, before amyloid and tau build up in the brain.
Cummings et al.
- Research article
- Peer reviewed
- Randomized
- Clinical trial
- People