A study shows that changes in the gut microbiome can identify people at risk of developing Parkinson's disease
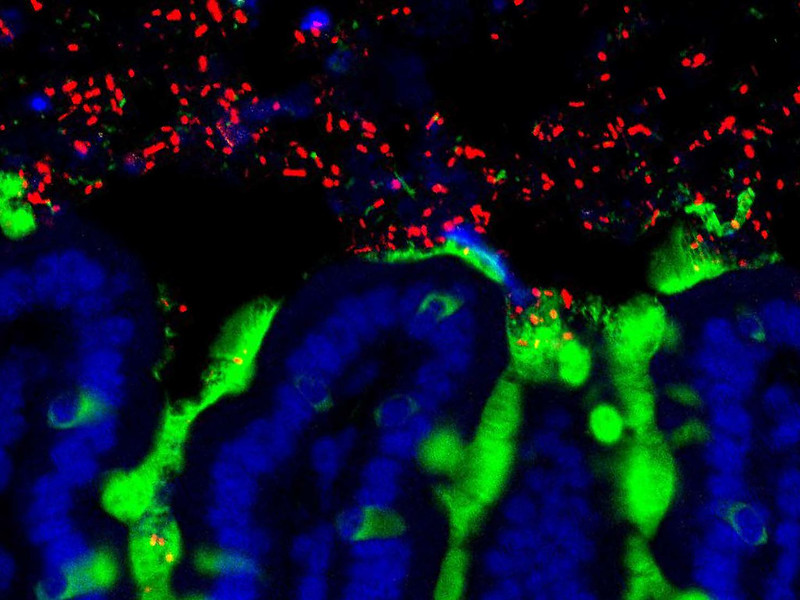
One of the best-known genetic risk factors for developing Parkinson’s disease is carrying variants of the GBA1 gene. A new study published in the journal Nature Medicine compared the microbiomes of 43 carriers of this gene who had not developed the disease with those of 271 Parkinson’s patients and 150 healthy individuals. The results showed, in addition to alterations in the microbiome in the patient group, that 25% of the microbiome of carriers of this gene exhibited alterations, representing an intermediate profile between the other two groups. The results were validated using independent cohorts from the United Kingdom, South Korea, and Turkey. According to the authors, “alterations in the gut microbiome can identify individuals with both genetic and non-genetic risk in the general population who may be progressing toward Parkinson’s disease.”