Clínic Hospital
If you are the contact person for this centre and you wish to make any changes, please contact us.
Head of the Cardiology Department at the Hospital Clínic de Barcelona and researcher at the National Centre for Cardiovascular Research (CNIC) and at the August Pi Sunyer Biomedical Research Institute (IDIBAPS)
Consultant in the Department of Preventive Medicine and Epidemiology at Hospital Clínic, University of Barcelona
Neurologist at the Hospital Clínic in Barcelona
Head of Microbiology at Hospital Clínic in Barcelona, associate professor at the University of Barcelona, and researcher at ISGlobal Barcelona
Psychiatrist and researcher at the Bipolar and Depressive Disorders Unit of the Hospital Clínic de Barcelona
Head of the Arrhythmias and Physical Activity research group at IDIBAPS, cardiac electrophysiologist at Hospital Clínic Barcelona, associate professor of Medicine at the University of Barcelona and researcher at CIBERCV.
Professor of Psychiatry at the University of Barcelona, Head of the Psychiatry and Psychology Department at Hospital Clínic in Barcelona, and researcher at the Biomedical Research Centre in Mental Health (CIBERSAM)
Neurologist at the Neuroimmunology Unit of the Neurology Department at Hospital Clínic de Barcelona
Psychiatrist and researcher at the Depressive and Bipolar Disorders Unit of the Hospital Clínic de Barcelona
Assistant Doctor of Psychiatry and postdoctoral researcher at the Bipolar and Depressive Disorders Unit of the Psychiatry and Psychology Department of the Hospital Clínic de Barcelona.

In 2023, 1.17 billion people suffered from a mental health disorder, compared to 599 million people in 1990, according to a global study published in The Lancet. Women experienced higher rates of anxiety and depression, while neurodevelopmental and behavioral disorders—such as ADHD or autism—are more common in men. The highest incidence was observed among those aged 15 to 19, which, according to the authors, underscores the need for early prevention and targeted support for this age group.
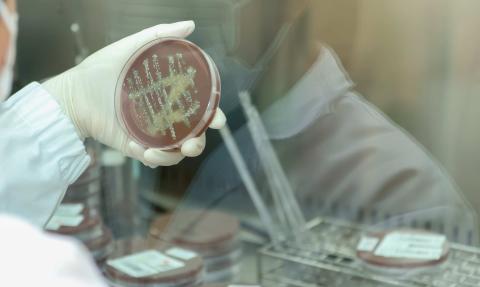
The latest reports from the European Centre for Disease Prevention and Control (ECDC) indicate a rise in bacterial sexually transmitted infections (STIs) across Europe. In 2024, notifications of gonorrhoea and syphilis, along with congenital syphilis, reached their highest levels in more than a decade, reflecting sustained transmission across multiple countries. Gonorrhoea has increased by more than 300 % over the past 10 years, with Spain among the countries with the highest rates, while syphilis has risen by around 100 %, with Spain also ranking second highest. Men who have sex with men are the most affected population group for both infections. Congenital syphilis increased by almost 250 %, described as “one of the most concerning findings” by two ECDC experts during the briefing presenting the results. Possible contributing factors include reduced condom use, an increase in sexual partners, as well as higher levels of testing.
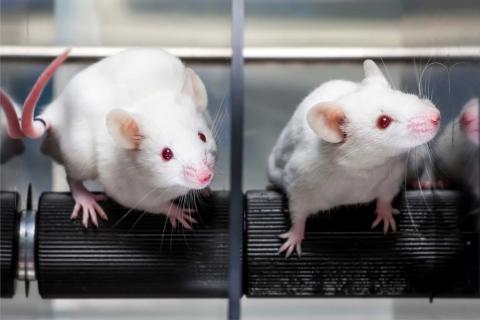
The eyes are connected to the brain via the retina, which makes it a potential pathway for brain stimulation. A study published in Cell Reports Physical Science has used contact lenses equipped with a system for transcorneal electrical stimulation to treat depression in animal models of the disorder. Mice fitted with the device showed behavioural improvements, including increased sociability, as well as physiological changes, such as the restoration of altered neural connections. The results were comparable to those obtained with fluoxetine —known commercially as Prozac— administered for three weeks in one of the mouse groups.
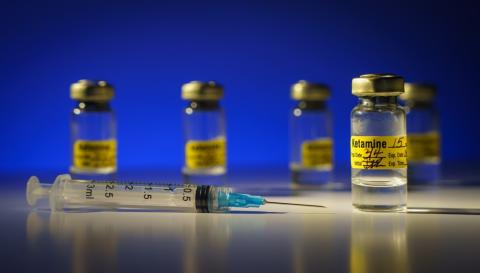
Single and repeated intravenous ketamine infusions are effective in reducing suicidal and depressive symptoms in patients with an acute episode of major depression. These are the main conclusions of a systematic review and meta-analysis published today in the journal JAMA Psychiatry, which also notes that long-term outcomes are not well established.

The Ministry of Health has announced that Spain will receive the MV Hondius in the Canary Islands “in accordance with international law and the spirit of humanitarianism”. The government is thus responding to a request from the World Health Organisation (WHO) and the European Union for the cruise ship, which is travelling from Argentina and has an outbreak of hantavirus on board, to dock in the Canary Islands, in the port of Granadilla, Tenerife. The European Centre for Disease Prevention and Control has assessed which passengers should be evacuated from the ship to Cape Verde, where it is currently located, and which will continue on to the Canary Islands. Once there, they will be examined and transferred to their home countries in accordance with safety protocols. The cruise ship is expected to arrive in the archipelago in three or four days.

The hallucinogen psilocybin, found in certain mushrooms, is being investigated as a treatment for conditions such as depression. A study published in Nature Communications shows that a single 25 mg dose of the compound can produce brain changes lasting up to a month after administration. These were measured using neuroimaging techniques in 28 healthy adults who had never taken psychedelics. In terms of psychological effects, participants showed increased cognitive flexibility, psychological insight, and well-being after one month.

A review published in The Lancet Psychiatry has examined the prevalence of major depressive disorder during pregnancy, the peripartum period—immediately before and after childbirth—and the postpartum period—up to twelve months after childbirth. The study, which used data from more than two million women and girls aged 10 to 59 from all regions of the world, showed that approximately one in 15 (6.8%) is affected by major depression during the year following childbirth and that the prevalence was highest during the first two weeks after childbirth (8.3%). The authors call for greater integration of screening, prevention, and treatment of this disorder during the peripartum period into current care models.
One of the best-known genetic risk factors for developing Parkinson’s disease is carrying variants of the GBA1 gene. A new study published in the journal Nature Medicine compared the microbiomes of 43 carriers of this gene who had not developed the disease with those of 271 Parkinson’s patients and 150 healthy individuals. The results showed, in addition to alterations in the microbiome in the patient group, that 25% of the microbiome of carriers of this gene exhibited alterations, representing an intermediate profile between the other two groups. The results were validated using independent cohorts from the United Kingdom, South Korea, and Turkey. According to the authors, “alterations in the gut microbiome can identify individuals with both genetic and non-genetic risk in the general population who may be progressing toward Parkinson’s disease.”
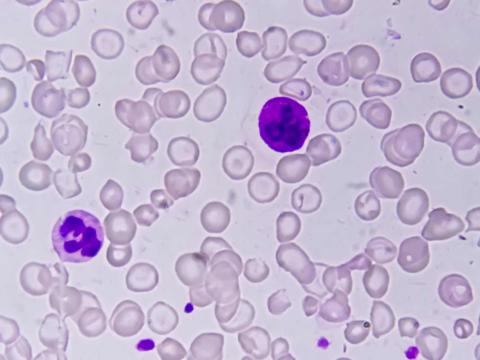
For the first time, CAR-T cell therapy has been used to treat a patient with three different autoimmune diseases – autoimmune haemolytic anaemia, immune thrombocytopenia and antiphospholipid syndrome – which were life-threatening and had resisted years of treatment. The patient, who previously required daily blood transfusions, has been in remission for a year without the need for further treatment since then. The case report, published in the journal Med, suggests that these therapies may help treat complex and severe autoimmune diseases.

Individualised dosing of a synthetic inhalable formulation of mebufotenine, a psychedelic substance, led to improvements in depressive symptoms compared with placebo and was well tolerated. These are the results of a phase 2 clinical trial published in the journal JAMA Psychiatry, which includes Spanish participation. According to the authors, this supports its potential as a novel, fast-acting treatment for treatment-resistant depression.